
Recognizing that health policy is one of the strongest indicators of positive health comes in marginalized communities is the golden ticket to health equity for all."
Rasheera D. Dopson Tweet
In the words of the late Dr. Martin Luther King Jr, he says “Of all forms of inequality, injustice in healthcare is the most shocking and inhumane.” Within the past two presidential administrations, we have seen the institution of healthcare be turned into an ongoing debate. Is healthcare a right or a privilege? While some may argue that healthcare is a privilege —only accessible to individuals who have proven themselves to be law abiding, hard working citizens. Some also view that healthcare is a right—granted to an individual not based on any merit or status but simply out of a need for humane and decent care. Nevertheless, to those who identify and live-in marginalized communities- healthcare is neither a right nor a privilege but it is a necessity.
The powerful words of Dr. King transcended the political landscaping of our healthcare system and got to the heart of the matter. Healthcare may be a right and a privilege to some, but it is neither if it’s not accessible to those who have it. In looking at the framework of health equity and its impact on marginalized communities, we in the field of public health have made tremendous strides in identifying and addressing the social determinants of health (SDOH). Within sectors of our public healthcare system, we also understand that these SDOH are amplified at the intersection of these marginalized communities. Those who fall within the intersection of Race, Gender and Disability remain vulnerable to these health inequities; often times falling between the cracks of our challenged healthcare system.
However, the SDOH of health that we do see in our communities do not serve as stand alone events or occurrences. Many of the SDOH are impacted by greater political influences that keep certain inequities in place. Hence, perpetuating cycles of negative health outcomes in marginalized communities. In overcoming and addressing these widespread health disparities, a more sustainable solution has to be put in place. In taking a systemic view of our current healthcare system—in order to reduce or eliminate the present-day inequities; we have to first acknowledge the decision-making power that rest behind the scenes enfolding our healthcare system.
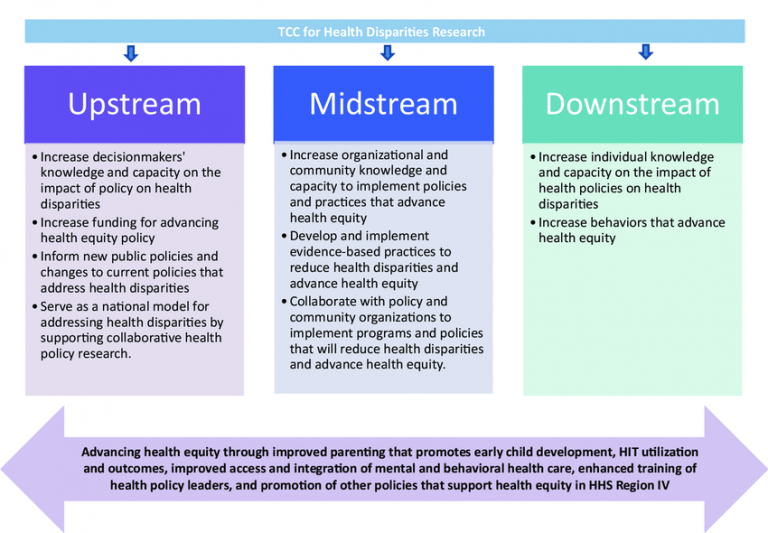
When observing the Political determinants of health (PDOH) the framework of Attorney Daniel Dawes comes into play. He examines the political decisions that lead to our social conditions. Within this framework Dawes also parallels to the McKinlay Model for Health promotions which illustrates three levels of policy intervention. In relation to our healthcare system these intervention levels will help in the establishment and support of an equitable healthcare system. One report reads “in a policy context health equity requires creation of the conditions necessary for people to achieve their optimal health potential.” The upward-downward stream model visibly outlines the driving force of the current health conditions we see in marginalized communities.
An example of this disparity was widely seen throughout the COVID-19 pandemic. Prior to the pandemic, many states had strict guidelines and regulations when it came to accessing telehealth services. Individuals who lived in digital deficit communities or rural areas face inequity in accessing healthcare systems. This was in large part due to policies set in place enabling patients from accessing more preventative services, such as individuals who were beneficiaries of Medicaid/Medicare benefits were uniquely marginalized. These individuals who were recipients of these services were limited in their use of telemedicine. It wasn’t until 2020 that these restrictions were lifted due to a policy change that enabled hundreds of thousands of individuals to access a readily available services. Although this is one example of a marginalized group being impacted by health policy change the results of their positive health outcomes are widely felt.
Recognizing that health policy is one of the strongest indicators of positive health comes in marginalized communities is the golden ticket to health equity for all. In alleviating problematic upward stream events – the downward impact can flow into a more positive and transformative direction that can change the health outcomes for vulnerable communities for generations to come.
More from Rasheera Dopson here.
HPHR.org was designed by ComputerAlly.com.
Visit HPHR’s publisher, the Boston Congress of Public Health (BCPH).
Email communications@bcph.org for more information.

Click below to make a tax-deductible donation supporting the educational initiatives of the Boston Congress of Public Health, publisher of HPHR Journal.![]()