
WHAT IS SO UNIQUE ABOUT INDIA’S NUTRITION AGENDA?
Multifactorial nature of malnutrition
Nutrition is not a standalone agenda. Given its multifactorial nature, nutritional outcomes are a result of policy actions across various sectors including health, development, agriculture, water and sanitation, which correlates with the integrated framework proposed for India’s revamped National Nutrition Mission called the POSHAN 2.0.6 Similarly, improved nutritional outcomes for the population, if developed within the framework of sustainable development, can simultaneously contribute towards achieving the multiple goals of supporting public health, local agri-food diversity, livelihood generation, women empowerment, and environmental sustainability.
To identify the contours of India’s nutrition agenda, it is critical to understand the scope of its nutrition burden. The term, malnutrition refers to deficiencies, excesses or imbalances in a person’s intake of energy and/or nutrients. Technically, malnutrition covers the double burden of ‘undernutrition’—which includes stunting (low height for age), wasting (low weight for height), underweight (low weight for age) coupled with micronutrient deficiencies and ‘overnutrition’- which includes overweight, obesity and diet-related non-communicable diseases (such as heart disease, stroke, diabetes and cancer).8 Moreover, malnourishment of mothers has scientifically shown to perpetuate a cycle of stunted growth within children, thus establishing the inter-generational impact of malnutrition on the health outcomes of the population.2 Finally, the economic rationale for investing in nutrition interventions has been well established; and the benefits-cost ratio for investing in community-based programs, anemia prevention, complimentary feeding, management of SAM children and providing micronutrient supplementation in India ranges anywhere between 6 to 50.5
India’s current nutrition profile
With a dedicated policy framework for nutrition, India has committed itself to achieving national and international targets to improve population level nutritional outcomes, along with an integrated approach to address the social determinants of nutrition, namely- health, sanitation, water security, age at marriage and family planning. The latest data from National Family Health Survey-5 (India’s DHS), so far released for 22 states and UTs, shows that while many states have shown an increase in exclusive breastfeeding and adequacy of diets, about half of the states have shown an increase in rates of stunting, wasting and underweight in children.7 To act upon the underlying determinants, we have to understand that indicators like stunting are multifactorial by nature. For example, stunting itself can be affected by variables like indicators of the mother a child is born to, economic situation of the household, adequacy of diets, water and sanitation facilities in the household, as well as interventions in nutrition promotion and health.
On the other end of the spectrum, NFHS-5 data also highlights an increasing trend for child obesity and impact of risk factors on development of chronic diseases in adults like hypertension and diabetes.7 This correlates with the modern realities of rapid urbanization and sedentary lifestyles, topped with the market influx of processed foods and refined carbohydrates.3 Moreover, what you put on your plate is fundamentally linked to its impact on the environment and climate change. To drive a transformational shift in this current scenario, the latest global evidence calls for building of resilient food systems, shorter supply chains, targeted food fortification and generation of local livelihoods that support dietary diversification, improved health outcomes, rural development and ecological conservation- all aimed at the achievement of UN-Sustainable Development Goals
Gap between knowledge to policy action
Global experience shows that it takes approximately 17 years to transfer research in to practice,1 which ultimately leads to tangible interventions on the ground. Similarly, in India there is no dearth of research and small-scale innovations that if translated accurately for policy action, can have a meaningful impact on population level outcomes. To address, this gap, it is critical to establish forums for knowledge translation which not only synthesise and disseminate the existing evidence base but also incubate outcome driven solutions that are scalable, sustainable and contextual.

WHAT IS KNOWLEDGE TRANSLATION AND WHAT ARE SOME LEVERS FOR ACTION?
Knowledge Translation
To contribute towards government’s mission for achieving a “malnutrition free India”, there is an urgent need to promote knowledge translation forums that are evidence driven and aimed at addressing the triple burden of protein-energy malnutrition, micro-nutrient deficiencies and overnutrition, with participation from the policy makers, academia, practitioners and the private sector.
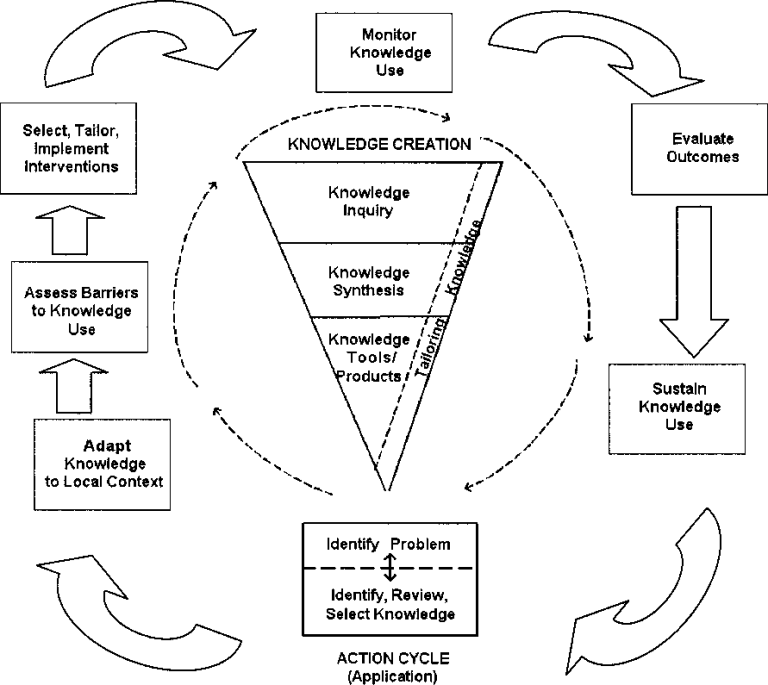
To conceptually appreciate the need for Knowledge Translation, the framework on “Knowledge to Action” process, as highlighted below is a relevant reference.4
Levers for Action
Public health and nutrition scientists are best placed to deploy the following levers for driving evidence in to action-
HOW TO ADDRESS THE GAP BETWEEN KNOWLEDGE TO ACTION FOR INDIA’S NUTRITION AGENDA?
Conclusively, the forum could serve both as an accelerator for knowledge translation to inform policy action and consumer behaviours, and as an incubator to test and promote solutions that are scalable, sustainable and contextual to India’s geography, population profile and socio-cultural diversity. Priority areas for collaborative action could include–
1. Balas, E. A., Boren, S. A., Bemmel, J., & McCray, A. T. (2000). Yearbook of medical informatics 2000: Patient-centered systems. Stuttgart, Germany: Schattauer, 65-70.
2. Black, R. E., Victora, C. G., Walker, S. P., Bhutta, Z. A., Christian, P., de Onis, M., Ezzati, M., Grantham-McGregor, S., Katz, J., Martorell, R., & Uauy, R. (2013). Maternal and child undernutrition and overweight in low-income and middle-income countries. The Lancet, 382(9890), 427–451. https://doi.org/10.1016/S0140-6736(13)60937-X
3. Cheng, A., Mayes, S., Dalle, G., Demissew, S., & Massawe, F. (2017). Diversifying crops for food and nutrition security–a case of teff. Biological Reviews, 92(1), 188-198.
4. Graham, I. D., Logan, J., Harrison, M. B., Straus, S. E., Tetroe, J., Caswell, W., & Robinson, N. (2006). Lost in knowledge translation: time for a map?. Journal of continuing education in the health professions, 26(1), 13-24.
5. Hoddinott, J., Alderman, H., Behrman, J. R., Haddad, L., & Horton, S. (2013). The economic rationale for investing in stunting reduction. Maternal & child nutrition, 9, 69-82.
6. Ministry of Women and Child Development. (2021). Initiatives to curb Childhood Malnutrition. https://pib.gov.in/PressReleasePage.aspx?PRID=1707478
7. National Family Health Survey, India (2020). Key Findings from NFHS-5. http://rchiips.org/nfhs/factsheet_NFHS-5.shtml
8. World Health Organization. (2020). Malnutrition. https://www.who.int/news-room/q-a-detail/malnutrition
HPHR.org was designed by ComputerAlly.com.
Visit HPHR’s publisher, the Boston Congress of Public Health (BCPH).
Email communications@bcph.org for more information.

Click below to make a tax-deductible donation supporting the educational initiatives of the Boston Congress of Public Health, publisher of HPHR Journal.![]()